Thyroid removal surgery: Overview, Indications, preparation, Procedure, side effects and results
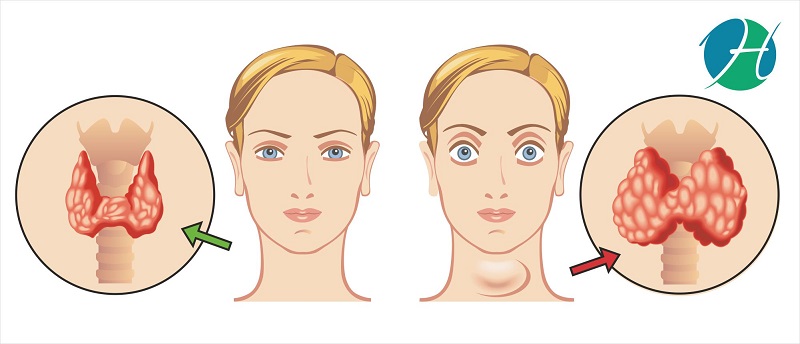
Thyroidectomy is the removal of a part or whole of the thyroid gland. Thyroid gland is a butterfly shaped gland located in the anterior part of the windpipe at the base of the neck which secretes hormones such as thyroxine in the blood. Thyroxine controls the basal metabolic rate of the body. Removal of thyroid is done to treat abnormality with the thyroid gland such as enlargement, cancer or overactive thyroid. The amount of gland to be removed depends upon the extent of abnormality and hence given various names to the surgery like partial or total thyroidectomy or lobectomy.
Indications
Thyroid removal surgery is recommended not only for cancerous causes but also for benign conditions. Following are the reasons for the removal of thyroid
- Thyroid cancer: It is the most common reason of removal of thyroid gland or thyroidectomy. Most of the thyroid cancer originates in the organ itself but rarely some cancer travel from other cancerous sites of the body to the thyroid gland too. If the cancer is located solely into the gland then only the gland part is removed. If it is spread to the nearby portions like lymph nodes and adjacent tissue. They need to be removed too.
- Goiter: It is enlargement of thyroid gland which is non-cancerous but the swelling of the anterior part of neck make it uncomfortable for the patient. It may cause difficulty in breathing by compressing action of swelling on the windpipe.
- Hyperthyroidism or overactive thyroid: in this disorder thyroid gland produces too much of thyroxine hormone. One of the treatment options for this condition is removal of that part of thyroid gland which is overactive. Sometimes the whole of the gland is abnormal and is removed completely.
- Thyroid nodules: these swelling comes to attention when noted by the patient, during a general physical examination or incidentally during an imaging procedure. Further tests are done to know the types of nodules. The treatment is advised depending upon the type of thyroid nodules. Cancerous or suspicious nodules are generally advised for the removal.

Risks
There are some risks associated with every surgery. Thyroid surgery is a safe surgery relatively but there may be some risks like
- Bleeding which may lead to airway obstruction.
- Infections
- Hypoparathyroidism which can be caused by damage to parathyroid glands. These glands are located at the back surface of the thyroid gland. Patients commonly complaints about numbness or tingling in different areas of body which is attributed to low levels of calcium in blood.
- Damage to nerves which control voice production resulting in permanent hoarseness of voice.
- Injury to the near structure like windpipe or food pipe.
The chances of risks and complications are lesser when performed by experienced surgeons.

Preparation
Most of the thyroid surgeries are elective. Therefore, the patients are well prepared for the surgery. Laboratory tests and various imaging tests need to be performed to see the extent of the area of thyroid gland involved. In patients suffering from the overactive thyroid gland, the production of hormone is made normal and the symptoms are decreased with the help of medications. Patients suffering from thyroid cancer may be advised to have prior radiotherapy treatment to shrink the tumor size.
As with all surgery requiring general anesthesia, the drug history of patient is checked and it is ensured that the patient is empty stomach for a few hours or a night before the surgery. The patient would be advised to take which medicines or not.

Procedure
Thyroidectomy is usually performed in general anesthesia. It means that the patient will remain unconscious throughout the procedure. The vitals of the patient like blood pressure, heart rate, respiratory rate and oxygen saturation are continuously monitored so that they remain at safe levels during the whole procedure.
After the patient becomes unconscious, the surgeon performs the surgery. Depending upon the abnormality and the situation of the patients there are several approaches to the surgery as
- Conventional thyroidectomy: in this approach the surgeon makes an incision in the center of the neck. It is the most common approach used.
- Endoscopic thyroidectomy: Small incisions are created in the neck through which surgical instruments and scope camera is inserted to perform the procedure. Endoscopic thyroidectomy can be performed through routes other than neck like axilla, mouth or even behind the ear approach.
- Robotic surgery: endoscopic thyroidectomy can also be done with the help of robotic assistance as well. It is more costly than conventional procedure. It has its own advantages and disadvantages depending upon the patient.

After surgery
After a successful surgery few people may experience side effects like pain in the area of neck and hoarseness in the voice which are often temporary. Pain can be relieved by medications for few days. In some patients, tubes may be inserted in the neck to drain the secretion which is removed later. The patient can resume drinking and eating after the surgery. Patient may stay overnight at the hospital or may go home the same day. The patient would be explained to take care of him or her
Results
The results will depend upon the patient’s diagnosis and the extent to which the surgery is done. For the patients who had undergone partial thyroidectomy don’t require thyroid hormone supplementation as the rest of the part of thyroid gland takes over the function. Patients having complete thyroidectomy need to take lifelong medications of thyroxine hormone. These are oral tablets need to be taken daily and patients would feel as comfortable as the people with normal thyroid glands. Routine follow up in these patients is done.

References
- Rogers-Stevane J, Kauffman GL Jr. A historical perspective on surgery of the thyroid and parathyroid glands. Otolaryngol Clin North Am 2008; 41:1059.
- Adam MA, Thomas S, Youngwirth L, et al. Is There a Minimum Number of Thyroidectomies a Surgeon Should Perform to Optimize Patient Outcomes? Ann Surg 2016.
- Nixon IJ, Whitcher M, Glick J, et al. Surgical management of metastases to the thyroid gland. Ann Surg Oncol 2011; 18:800.
- Haugen BR, Alexander EK, Bible KC, et al. 2015 American Thyroid Association Management Guidelines for Adult Patients with Thyroid Nodules and Differentiated Thyroid Cancer: The American Thyroid Association Guidelines Task Force on Thyroid Nodules and Differentiated Thyroid Cancer. Thyroid 2016; 26:1.
- Stang MT, Armstrong MJ, Ogilvie JB, et al. Positional dyspnea and tracheal compression as indications for goiter resection. Arch Surg 2012; 147:621.
- American Thyroid Association Guidelines Task Force, Kloos RT, Eng C, et al. Medullary thyroid cancer: management guidelines of the American Thyroid Association. Thyroid 2009; 19:565.
- Ross DS, Burch HB, Cooper DS, et al. 2016 American Thyroid Association Guidelines for Diagnosis and Management of Hyperthyroidism and Other Causes of Thyrotoxicosis. Thyroid 2016; 26:1343.
- Rosato L, Avenia N, Bernante P, et al. Complications of thyroid surgery: analysis of a multicentric study on 14,934 patients operated on in Italy over 5 years. World J Surg 2004; 28:271.
- Adam MA, Speicher P, Pura J, et al. Robotic thyroidectomy for cancer in the US: patterns of use and short-term outcomes. Ann Surg Oncol 2014; 21:3859.
- Grant CS, Stulak JM, Thompson GB, et al. Risks and adequacy of an optimized surgical approach to the primary surgical management of papillary thyroid carcinoma treated during 1999-2006. World J Surg 2010; 34:1239.

